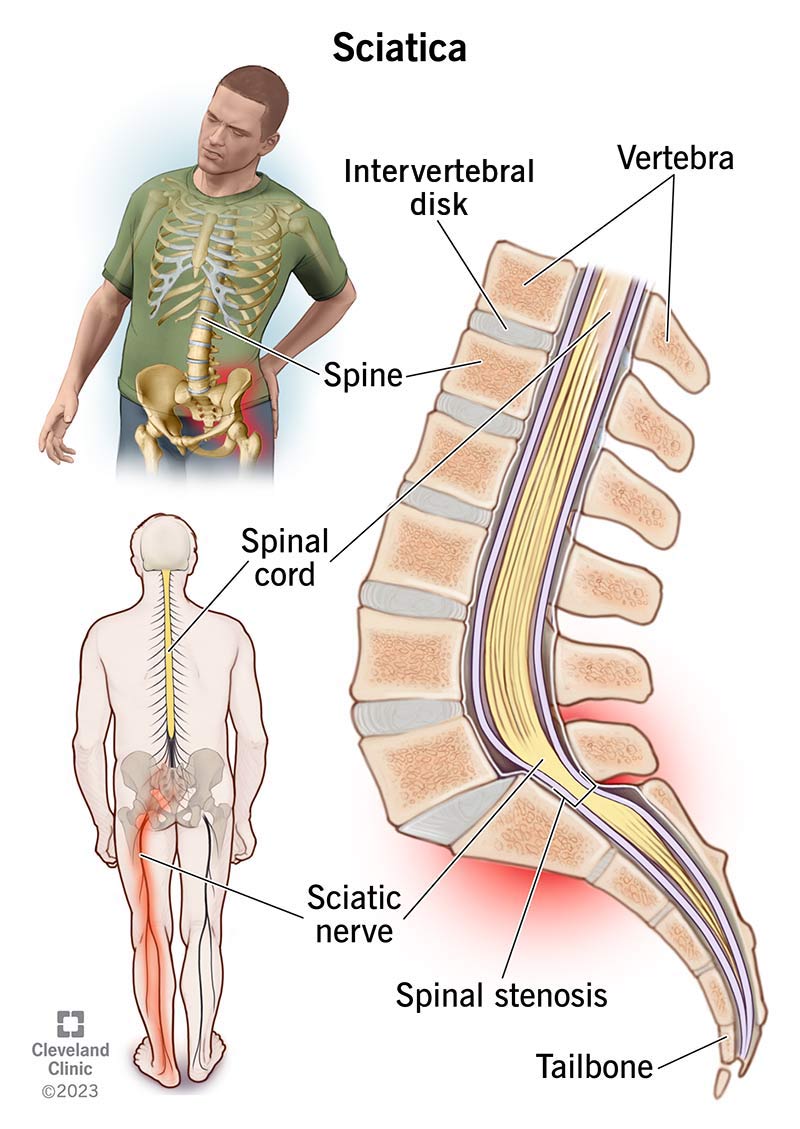
Sciatic nerve symptoms are commonly caused by:
- Herniated Lumbar Disc: Occurs when the nucleus pulposus (inner gel-like core) of an intervertebral disc protrudes through the annulus fibrosus (outer layer), causing chemical irritation to the adjacent nerve roots, most commonly at L4-L5 or L5-S1.
- Degenerative Disc Disease (DDD): An age-related or biomechanical process where intervertebral discs lose hydration and elasticity, leading to disc height loss, reduced shock absorption, and possible impingement of lumbar sacral nerve roots
- Lumbar Spinal Stenosis: A narrowing of the spinal canal or intervertebral foramen in the lumbar spine, often due to osteophyte formation, disc bulging, or ligamentum flavum hypertrophy, resulting in compression or impingement of the lumbar sacral nerve roots.
- Piriformis Syndrome: the sciatic nerve can be compressed or restricted by the piriformis muscle as it passes through the greater sciatic foramen, leading to similar nerve root or radicular symptoms down the leg. This is the least common mechanism of sciatic symptoms.
These conditions result in mechanical compression or chemical irritation (an inflammatory response ) of the nerve roots.
Patients with sciatica may present with:
- Radicular pain described as sharp, burning, or electric-like, radiating from the lumbar region through the gluteal area and posterior leg.
- Paresthesia or numbness in specific dermatomal patterns along the leg, depending on the particulate, particularly nerve roots affected.
- Motor deficits or weakness in dorsiflexion or plantarflexion, depending on the affected roots (Davis et al., 2014).
It is crucial for Pilates professionals working in rehabilitative settings to differentiate between musculoskeletal tightness and neural tension. One tool that can be used for this differentiation is the straight leg raise test (SLR).
To assess sciatic nerve irritability, the SLR is a foundational neurodynamic test.
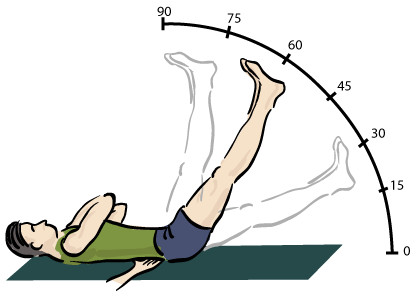
Procedure:
- Client position: Supine on a firm surface.
- Therapist action: Passively raise the patient's straight leg while maintaining knee extension.
- Observation: Monitor for symptom reproduction—pain, tension, or neurological sensations such as numbness, tingling or burning symptoms.
Positive SLR Criteria:
- Reproduction of clients radicular symptoms, while leg is positioned between 30°–70° of hip flexion
- Pain provocation below the clients knee , along the posterior leg aspect of the leg i.e. calf.
A positive test indicates sciatic nerve tension and/or inflammation, but does not diagnose the reason for sciatic symptoms. Further testing by a physician or skilled practitioner is needed for thorough diagnostics.
A negative test does not provoke these symptoms, helping to rule out significant neural involvement.
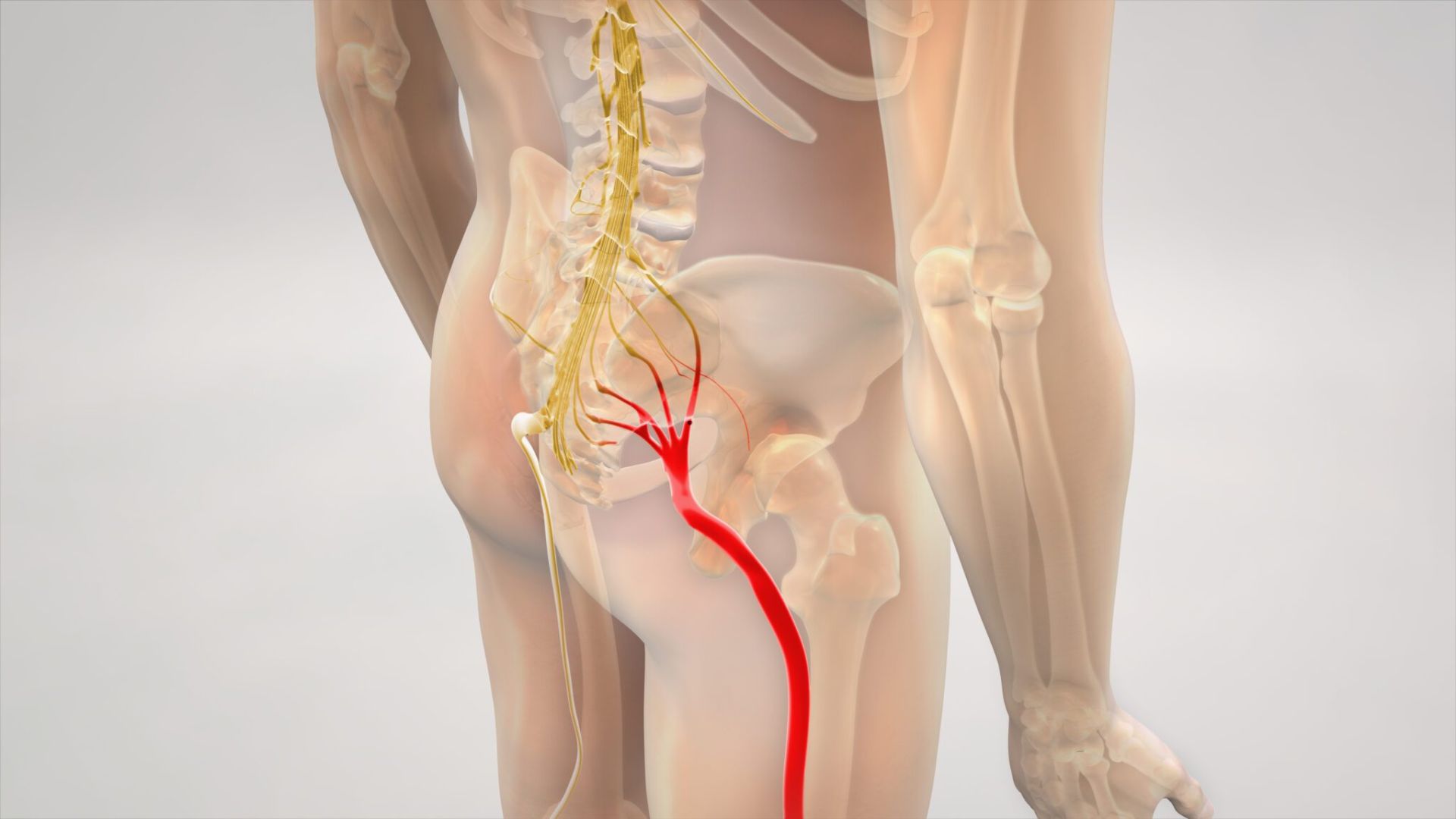
Understanding the irritability of the sciatic nerve is essential when designing or modifying a Pilates-based rehabilitation program. If the nerve is acutely inflamed or sensitized, excessive neural tensioning can exacerbate symptoms. Movements to avoid or modify include:
- Feet in straps (single or double leg), especially if hamstring lengthening is involved
- Hamstring stretching in any form
- Spinal flexion which may increase intradiscal pressure
- Screen for Neural Irritability: Use the Straight Leg Raise (SLR) test as a key assessment tool. When appropriate, consult with referring clinicians to ensure accurate interpretation and integration into your programming.
- Be Aware of Contraindicated Movements: Certain Pilates exercises should be avoided for clients experiencing sciatic nerve root symptoms (some mentioned above)
- Focus on Spinal Support: Incorporate neutral spine alignment and core stabilization exercises to minimize spinal disc stress and related nerve root irritation.
- Prioritize Movement Strategies: Emphasize pelvic-lumbar dissociation, and a gradual reintroduction of spine and hamstring mobility as symptoms subside.
- Understand Nerve Root Care: There are times when the sciatic nerve root needs protection, and times when it benefits from movement and neural flossing techniques. For a deeper dive into this clinical reasoning, explore my e-book and virtual course at Clinical Instructor Academy .
Understanding sciatic nerve tension is not just a clinical detail—it’s a crucial element of responsible, effective Pilates instruction. When instructors can recognize the signs of neural tension and modify exercises accordingly, they help protect clients from aggravating symptoms, support safe movement progressions, and build lasting trust.
Ultimately, this knowledge empowers instructors to work more holistically, addressing not just strength and flexibility but the nervous system’s role in movement and recovery. By deepening their understanding of sciatic nerve tension, Pilates professionals elevate both their expertise and their ability to truly change lives through movement.






